Ibogaine is a naturally occurring psychoactive substance found in the iboga plant of Western and Central Africa. Valued for its medicinal qualities, as well as for its spiritual and ceremonial role in the Bwiti religion, ibogaine has been used for centuries by the Fang, Mitsogo, and Punu peoples of Gabon and the Congo Basin.(1)
In recent decades, ibogaine has been making waves as a potentially revolutionary medication for addiction treatment. The modern era of ibogaine research dates back to the early 1960s, with the number of studies increasing throughout the 1990s and 2000s. (2)
Ibogaine’s potential use in the tempering of withdrawal symptoms from addictive substances such as cocaine and opioids has made it an important compound for research, development, and implementation. It also has a long history of providing rewarding journeys for psychedelic practitioners. The ibogaine experience is said to be unlike anything else, and its use can lead to profound introspection and personal growth. (3) (4)
What is Ibogaine?
Keep Up with Uncensored Psychedelic Trends
Join our newsletter at Psychedelics Uncensored.
We respect and protect your privacy. By subscribing your info will be subject to our privacy policy . Unsubscribe easily at any time
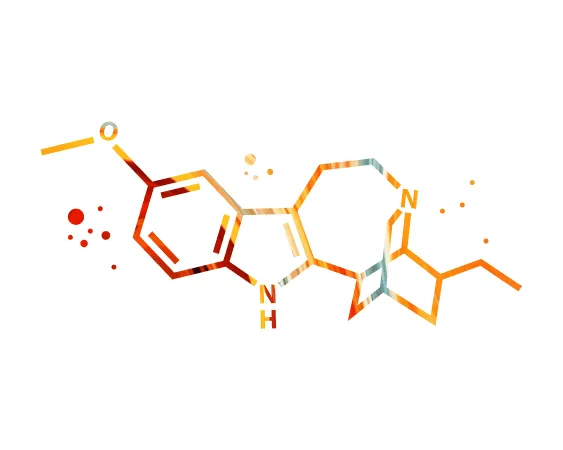
Ibogaine (12-methoxyibogamine) is a psychoactive indole alkaloid found naturally in the evergreen shrub Tabernanthe iboga or simply iboga. The highest concentration of ibogaine can be found in the root of the iboga plant, with mild potency in the rest of the plant. The root bark contains 6% of indole alkaloids, including ibogaine, ibogaline, ibogaine, and tabernanthine, 80% of these belonging to ibogaine.(5, 6, 7)
The iboga shrub is native to Central Africa and parts of West Africa. It has been used for centuries in ceremonial practices, notably in the Bwiti religion of Gabon, as a right of passage for young males. (5)
Ibogaine became more widely researched in Western medicine during the 1990s and the iboga plant’s therapeutic and psychoactive properties have gained notoriety for their “anti-addictive” properties. Anecdotal evidence and self-reports have shown that 6-25mg/kg of ibogaine has been reported to reduce both physical dependence and withdrawal symptoms for opiates, alcohol, psychostimulants, and nicotine.(5)
While the ibogaine alkaloid has shown promise in treating symptoms of substance use disorders (drug addictions), clinical trials remain difficult to facilitate, due largely to complications around ibogaine’s legal status.
Beyond its religious and medical uses, the recreational and spiritual use of ibogaine is practiced in Africa and other parts of the world, though not as widely as psilocybin or other classic psychedelics. Due to its potency and potential for emotional distress, it is recommended that those taking ibogaine do so in a controlled setting with an experienced guide, sitter, or integration coach present. There are also reported cases of ibogaine leading to health complications in certain individuals, notably those with heart conditions. A full medical screening by a healthcare provider should be performed before taking ibogaine, as well as having a medical professional present during the experience.(3) (4) (8) (9)
The Ibogaine Experience
How people experience ibogaine will primarily depend on the dose taken. Small amounts of ibogaine can create a mild stimulant effect which increases alertness. Larger doses, known as a “flood dose”, often produce an oneiric or “dream-like” state and is often the desired experience when taking ibogaine.(3) (9)
Keep Up with Psychedelic Trends
Get uncensored psychedelic news, events, and updates. Join Psychedelics Uncensored!
We respect and protect your privacy. By subscribing your info will be subject to our privacy policy . Unsubscribe easily at any time

Some users have described this oneiric state as a sensation of deep introspection and agency in one’s thoughts, that may include ethereal closed-eye visuals. Open-eye visuals have also been reported, such as tracers and light sensitivity, though closed-eye visuals are the most common occurrence. (5) (10)
The ibogaine experience lasts much longer than other psychedelics. Acute effects of ibogaine begin 1-3 hours after it is ingested and begins to metabolize. The first 3-12 hours are often intense and include rapid cyclical thoughts, rapid imagery, auditory hallucinations, and insomnia. Users will often experience the peak of ibogaine’s effects between 8 and 20 hours, with residual effects lasting up to 72 hours. Anecdotal reports have suggested that some people may feel the effects of ibogaine for up to 96 hours after ingesting. Ibogaine’s powerful effects have led it to be dubbed the ‘stern father’ of psychedelics. (11) (12)
In 2015, Kevin Franciotti, a journalist and then heroin addict, visited an ibogaine treatment center and detailed his ibogaine experience for MAPS, who were conducting a study on ibogaine’s effectiveness for addiction treatment in a clinical setting. Franciotti describes the height of his ibogaine experience, saying:
“I remember what I was told to expect before the medicine took effect. Upon this realization, I realize that this is going to be quite an experience. Moments later, while I’m lying on my side with my eyes closed, I feel an intense rush of energy that pulsates throughout my body. Immediately I understand why it’s called a “flood dose.” My body feels washed in a cleansing energetic blanket that completely removes the physical discomfort I’m feeling after 36 hours without heroin. In my mind, there’s a vision like I’m being launched through a worm-hole which spits me out in what looks like outer space. I’m having a very rapid succession of incredibly insightful thoughts and ideas, and I’m broadly contemplating various abstract concepts such as relativity theory, evolution, and photosynthesis.”
Franciotti goes on to illuminate the rest of his experience with ibogaine and how it helped to reduce the symptoms of his dependence on heroin. The above experience shares commonalities with other anecdotal reports of ibogaine and those who partake in ibogaine treatments. Some seeking addiction treatment have promoted the substance’s ability to leave users with long-lasting emotional and cognitive benefits. (13)
Preparing for Your Ibogaine Treatment
As with other psychedelic substances, one of the most crucial elements to prepare for a positive ibogaine treatment is having respect and an understanding of it. Ibogaine creates a powerful experience that can be incredibly fulfilling, and proper preparation and knowledge before diving in will ensure the best results.

A core principle of a comfortable and rewarding psychedelic journey is “set” and “setting.” These two components focus on the individual and their state before taking ibogaine (set) and the surroundings they choose to do it in (setting).
Set considers the individual’s mental state, their intentions, and how prepared they are for the experience. Setting is about the experience outside of yourself and refers to the environment you are in, including sensory considerations such as smells, music, and how the space you are in is decorated.(9)
Unlike classic psychedelics, which can be taken without clinical supervision, ibogaine’s powerful effects and complex side effects warrant consumption in a controlled environment. Most ibogaine treatment patients, especially those seeking addiction treatment, will do so at a clinic, where preparations are generally taken to ensure the individual is ready for the experience, the setting is comfortable, that sensory interferences such as light and sound have been considered, and that all safety measures are being upheld.(9)
What to Expect During Your Ibogaine Treatment
An ibogaine treatment can be encapsulated by its intensity, duration, and unique neurological effects. The exact nature of the experience is difficult to classify as most people struggle to qualify what it felt like afterward. One small study found that 90% of its participants had a trouble recalling details of their experiences with ibogaine. (14)
Despite the difficulty in recalling specifics about the experience, anecdotal and observational accounts suggest an ibogaine treatment begins with an intense onset period, characterized by rapid imagery, thoughts, and audible hallucinations. This point in the experience may be uncomfortable for some, so it is crucial to get your set and setting right beforehand. This phase will eventually give way to immersive and detailed closed-eye visual hallucinations that may be particularly vivid. This is often coupled with a deep level of introspection and self-reflection that can be incredibly clarifying. (3) (12)
The onset of effects during an ibogaine treatment is usually noticeable within 1-3 hours of administration and residual effects can be felt for up to 72 hours. The duration of effects and their intensity are broken up into 3 phases: acute, evaluative, and residual stimulation. However, the individual may not be able to discern a clear difference between phases during the actual experience. (12)
Integrating Your Ibogaine Treatment
Incorporating important reflections, meaning, and lessons from psychedelic journeys into daily life is an important step for most people. This process, known as integration, is work done by an individual or with the help of an integration coach after a psychedelic experience. The specific steps of integration can vary for everyone and are often different for those trying to integrate an ibogaine treatment. (15)(16)
Ibogaine treatment, integration specialist, and Psychedelic Program Coordinator for the Center for Optimal Living Juliana Mulligan describes integration as “a process of figuring out what the messages, lessons, and takeaways from the psychedelic experience were, and figuring out how to apply those to your daily life… It’s also about processing all the underlying emotional stuff that gets brought up by the psychedelic experience.” (17)
While it is advised to speak to an integration coach or specialist to get the most out of the process, these steps can help with your ibogaine integration.
01
Talk to a professional: As mentioned, an integration coach can help focus the process and give valuable insight into making lasting changes. It is also beneficial to speak to a therapist, counselor, or other psychological professional. (18)
02
Keep a journal: A big part of integration is paying attention and noticing any changes or differences in your psyche after a psychedelic experience. Keeping a journal can help document and keep a record of these changes. (17)
03
Looking after physical health: Taking care of your body can include exercise, healthy nutrition, getting enough sunlight, and avoiding unhealthy habits. (15)
04
Practice mindfulness: Yoga, meditation, and breathing exercises can all help you to recenter yourself and better integrate the experience.
05
Create daily routines: Adding insights or lessons into your daily routine is the central goal of integration. Creating daily rituals and routines that incorporate these insights can help with this process.
As mentioned, integration is a unique process and can be different for everybody, so approach it in the way that is most beneficial for you. The Modern Psychedelics podcast interview with Lana Pribic details her experience with iboga and integration process, showing that there are various ways to achieve integration.
Potential Benefits of Ibogaine Treatments
Psychotherapeutic applications
Since the 1960s ibogaine has been studied for its potential to reduce cravings for certain psychoactive substances, with studies also showing its potential for treating certain mental health conditions. Open-label studies and observational reports from ibogaine treatment clinics have shown that ibogaine can reduce withdrawal symptoms from certain substances. A recent study has also shown that ibogaine, when combined with magnesium to protect the heart, may safely and effectively reduce symptoms of PTSD, anxiety, and depression in military veterans with Traumatic Brain Injury. (19) (20)
The bulk of ibogaine research, however, remains focused on addiction and substance use. Studies have shown a low dose of ibogaine (10-12mg per kg of body mass) can decrease withdrawal symptoms from opioids, opiates, and stimulants such as cocaine or methamphetamine. One study showed that of 75 participants who had a substance use disorder, 61% remained abstinent from substance abuse for over a year. (21) (22)
While this study saw no fatalities or adverse reactions, there have been concerns raised by other research into ibogaine’s effect on the heart. Most research into the cardiac toxicology of ibogaine points to heart arrhythmias, some instances resulting in fatality. Research also suggests that ibogaine’s potential as a life-saving treatment for substance use disorders means its application should still be conducted after a full risk assessment deems it safe to do so. (23)
Personal Growth
Some iboga and ibogaine therapeutic retreats offer treatment programs dedicated to personal growth. Beond, an ibogaine treatment center in Cancun, Mexico offers programs that are distinct from those designed to treat addiction and mental health and can be tailored to meet an individual’s specific needs through tailored workshops. These workshops can help with self-awareness, exploring spiritual beliefs, integration coaching, and long-term personal growth planning. (24)
Anzelmo, another Mexico-based treatment center promotes the psychospiritual benefits of ibogaine use, suggesting treatment helps with “cultivating awareness of the self and its relationship both to the human collective, personal ancestral roots, and to nature.” While individual centers report ibogaine’s benefits to personal growth, there has been little scientific investigation outside of its application in substance use disorder treatment or mental health conditions. (25)
History & Cultural Relevance of Ibogaine
Ibogaine and the iboga plant have a long and rich history that spans centuries, with applications in cultural, religious, and medicinal practices. From its roots in ceremonial practices in Central Africa to pioneering treatment for substance use disorders, ibogaine has held an important place in the history of psychedelics and plant medicine.
Gabon and the Bwiti Religion

The use of the iboga plant in religious, ceremonial, and medicinal practices can be traced back centuries in parts of Western-Central Africa, notably in Gabon and with the Fang, Mitsogo, and Punu peoples of the Congo Basin. Its use became more widespread at the turn of the 20th century through the Bwiti religion. (1)
Bwiti followers use the iboga plant in ceremonial practices and as a right of passage for young males. When a young male (between 9 and 12 years old) is deemed ready, they are given a larger “flood dose” of Iboga root, which contains the highest concentration of ibogaine. They are then sent away to experience their ibogaine journey with the intention of communing with their ancestors. (26) (27)
This practice, believed to be adopted from an older religion known as Byeri, who used the alan plant in the same context, has since been adopted by groups outside of Gabon. The Fang, a group who populate large parts of Central Africa, have taken Bwiti iboga practices further into parts of the Congo and Cameroon. (27)
Western Discovery of Ibogaine
Western awareness of ibogaine occurred in the mid-19th century when French and Belgian colonists witnessed iboga ceremonies for the first time in Africa. The earliest documentation of the iboga plant was by ethnobotanist Griffon du Bellay in 1865, and in 1885 it was officially classified by Father Joseph-Henri Baillon. Ibogaine was first isolated in 1901 and was marketed as a stimulant in France in the 1930s. (28) (29)
Early Use of Ibogaine Treatments
By the 1960s, ibogaine had made its way across the Atlantic, and the roots of its potential for substance use disorder treatment began to form. Howard Lostof, who went on to pioneer ibogaine treatment for substance use disorders, was first introduced to it in 1962. Suffering from heroin dependency at the time, a chemist friend gave him some ibogaine, and after taking it, he realized he had experienced days without heroin with no withdrawal symptoms. (30)
He later described feeling released from the fear and anxiety that held him in his dependency. He conducted his own trials on those with heroin dependency, and of the seven people he gave ibogaine to, five reported not feeling the need to use heroin for six months or longer, leading Lotsof to dub ibogaine an “addiction disrupter.” As with other psychedelic researchers of the time, Lotsof’s pioneering work with ibogaine was cut short when the United States Food and Drug Administration (FDA) classified ibogaine and other psychedelics as Schedule 1 substances under the Controlled Substance Act (CSA) in 1970. This forced Lotsof and other psychedelic therapists underground to conduct trials in secret. (31, 32, 33, 34, 35)
Underground Research and Future Potential
Further research into ibogaine’s potential for dependency treatment was slowed considerably after the Controlled Substance Act came into effect and remained low throughout the 1970s.(36)
Lotsof, along with his wife Nancy and other collaborators, continued to campaign for ibogaine research while conducting trials in secret throughout the ‘80s with little interest from pharmaceutical companies or government agencies. In 1985, Lotsof patented the ibogaine molecule for the purposes of addiction treatment, but could not get his treatment approved.(37) (24)
In 1987, the first international Conference on ibogaine was held, bringing together researchers and advocates from around the world. The first human experiments were conducted around the same time in Holland, and Dr. Stanley Glick’s research into ibogaine treatment for rats with morphine dependence showed promise.(37) (38)
In the early ‘90s, Lotsof and Dr. Debora Mash managed to push for FDA permission to begin human trials following a 40% efficacy rate from a trial conducted in Holland. The FDA approved it, but the National Institute on Drug Abuse (NIDA) did not. Progress was further disrupted when Dr. Mark Molliner published a report showing that ibogaine caused neurotoxicity in rats. This report was widely debunked as Dr. Molliner had prescribed the rats five times the rate of ibogaine used in previous dependency trials, but this did not stop the media from widely discrediting ibogaine research. (36) (37)
NIDA associate director Dr. Frank Vocci would bring a full stop to proceedings in the mid-’90s when he halted all trials, including animal trials, and decreed that no public funds would be used for ibogaine research again. Treatment once again went underground in the U.S., and unregulated treatment centers began to appear around the world. Some of these treatment centers have performed observational studies (in Mexico and New Zealand), and in 2021 clinical trials for opioid withdrawal treatment were approved in the UK. (36) (37)
Interest in ibogaine research has recently increased in the U.S.. In 2023, The Kentucky Opioid Abatement Advisory Commission revealed plans for $42 million to be spent on funding research and trials into ibogaine treatment for substance abuse. Note: Due to changes in local Kentucky government policy, this program for ibogaine funding may be delayed or dismantled. (39) (40)
Is Ibogaine Legal?

Ibogaine has a complex legal status around the world, being illegal in much of the Western hemisphere, legal in other countries due to its medicinal properties, and having complex laws in others. In some countries, the legal status is classified as “unknown,” meaning there are no set laws for ibogaine. Dedicated treatment centers exist around the world, though many operate underground due to ibogaine’s legal status and medical concerns. (41)
Countries Where Ibogaine is Illegal
| FLAG | COUNTRY / STATE | LAWS |
|---|---|---|
| 🇺🇸 | United States | Since the inception of the Controlled Substance Act in 1970, ibogaine has been classified as a Schedule I substance, making it illegal to distribute or possess the substance. This means that within the U.S., there are currently no legally operated ibogaine treatment centers.(41) |
| 🇬🇧 | United Kingdom | The UK released its much-derided Psychoactive Substance Act in 2016, making it illegal to produce and distribute ibogaine. However, the bill means possession is still legal though buying it would still be a crime. (41) |
| 🇫🇷 | France | Possession and distribution are completely illegal in France, despite it being one of the first countries to market ibogaine commercially in the 1930s. (41) |
| 🇮🇪 | Ireland | Ireland’s Psychoactive Substance Act makes most psychedelics illegal to possess or distribute. A clause regarding medicinal trials and development could mean ibogaine trials will be possible there. (41) |
| 🇧🇪 | Belgium | One of the few countries to have banned ibogaine by Royal Decree, the substance has been illegal since 1998. Ibogaine treatment will be very hard to come by in Belgium. (41) |
| 🇸🇪 | Sweden | Sweden has outlawed the possession and distribution of ibogaine since 1985. (41) |
| 🇮🇹 | Italy | Ibogaine was recently added to the country’s Schedule I drug classification, making possession and distribution illegal. (41) |
Where Is Ibogaine Legal or Unregulated?
| FLAG | COUNTRY / STATE | LAWS |
|---|---|---|
| 🇲🇽 | Mexico | Mexico has been a popular destination for ibogaine treatment since the late 1980s, owing to the substance’s unregulated status. Ibogaine treatment centers in Mexico should be well-researched before attending. (41) |
| 🇧🇷 | Brazil | Ibogaine is legal in Brazil and has recently been allowed for monitored medical treatment in São Paulo. (41) |
| 🇵🇹 | Portugal | Possession and distribution are completely illegal in France, despiteIn 2001, Portugal decriminalized many psychoactive substances, including ibogaine. Distribution remains a gray area, and treatment centers are not commonplace. (41) it being one of the first countries to market ibogaine commercially in the 1930s. (41) |
| 🇨🇷 | Costa Rica | Costa Rica is internationally renowned as the place to go for ibogaine treatment owing to its long-standing legal status. It is still advised to do research into treatment centers before going, as the popularity has led to illegitimate ibogaine retreats cropping up. (41) |
| 🇬🇦 | Gabon | Gabon is the birthplace of ibogaine use, and governmental laws protect its use and the iboga plant. (41) |
| 🇬🇹 | Guatemala | Ibogaine’s law is unclear in Guatemala though there are many ibogaine treatment centers that operate in the city of Antigua. (41) |
| 🇳🇱 | Netherlands | Ibogaine is not prohibited in The Netherlands. There are several ibogaine treatment centers in the country. (41) |
| 🇳🇿 | New Zealand | Ibogaine treatment and prescription have been legal in New Zealand since 2009, and many treatment centers provide ibogaine treatment for substance use disorders. (41) |
| 🇿🇦 | South Africa | Ibogaine treatment is legal in South Africa, provided the center or practitioner has a license. (41) |
Countries With Mixed Legality
| FLAG | COUNTRY / STATE | LAWS |
|---|---|---|
| 🇦🇺 | Australia | Ibogaine is technically a prescription-only medication in Australia. However, there are no laws against possession and cultivation, even without a prescription. (41) |
| 🇨🇦 | Canada | In Canada, individuals are allowed to use and possess iboga and ibogaine legally for personal purposes. However, in 2017, Health Canada placed ibogaine on the Prescription Drug List (PDL), which means that it can only be legally acquired with a prescription from a medical provider. (41) |
| 🇩🇰 | Denmark | Ibogaine has been illegal in Denmark since 1993, though special permission from the government for drug trials is common in the country, meaning ibogaine research is possible.(41) |
| 🇫🇮 | Finland | Since 2014, it has been legal to possess ibogaine but sale, transport, and cultivation remain illegal.(41) |
| 🇺🇾 | Uruguay | Uruguay is one of the few countries to have never criminalized substances for personal use. Distribution and cultivation are still controlled, but penalties are left up to the judge in each case. (41) |
Access & Ibogaine Treatment Centers
Accessing ibogaine for substance use disorder treatment, mental health treatment, or to participate in a psychedelic journey will require visiting a country where the substance is legal and has dedicated ibogaine treatment centers or ibogaine retreats. There is also the option of participating in a clinical trial. Clinicaltrials.gov regularly updates trials that are actively seeking candidates for ibogaine research.
When looking for an ibogaine treatment center or retreat, it is important to do thorough research first. While many centers offer a full ibogaine experience complete with aftercare, safety measures, and accommodation, many instances of poor standard centers or scams have been reported. Knowing what to look out for when seeking ibogaine treatment can be difficult, as the requirements and standards a center should have vary from other psychedelic treatment centers. Some things to take note of when researching ibogaine treatment centers include: (42)
Ibogaine Treatment for Addiction
The promise of ibogaine as a treatment for withdrawal symptoms of substance use disorders has been well-studied for over half a century. From Lotsof’s initial underground trials in the ‘60s to observational studies in ibogaine treatment centers in Costa Rica and New Zealand, preclinical studies in animals have supported self-reports that ibogaine aids in both drug cravings and withdrawal symptoms. Studies have shown that ibogaine interacts with opioid and glutamatergic systems, which play a role in physical withdrawal.(43,44,45,46)
While ibogaine treatment has shown potential as an effective addiction treatment, progress in developing the substance as a viable option for substance use disorders has been hindered since its early study, though research and study have been increasing since the 1990s. (47)
There has also been scrutiny of the substances’ effect on the cardiovascular system and the risk of cardiac arrhythmias owing to ibogaine toxicity, which has been attributed to over 30 recorded deaths. These reports have emerged from several treatment centers around the world, as well as from studies into opioid withdrawal treatment. (43, 45, 48)
Microdosing Ibogaine
According to anecdotal reports, a microdose of ibogaine usually consists of 50-100mg capsules or 25mg concentrate and is sometimes referred to as a “hunter’s dose.” It is possible to function normally on this dose, and anecdotal reports suggest it can boost clarity and cognitive awareness which can be beneficial for some routine activities. It is also reported to boost appreciation of the world and increase rational sensitivity and empathy.(49)
Microdoses of ibogaine have also been used to research treatment-resistant depression. A 2022 study tested a 47-year-old female with bipolar type II who was experiencing a severe depressive episode. The participant, who was taking mood stabilizers and escitalopram 15 mg/day to treat her condition, was administered two capsules of high-purity ibogaine hydrochloride containing 4 mg of ibogaine each (approximately 1% of a full conventional single dose) over 60 days. (50)
Observers reported improvements in the participant’s condition, specifically regarding mental clarity, organized thinking, and positive prospects regarding the future. The participant also self-tapered off of her prescribed medication during the study (with the exception of alprazolam) and continued to show improvement in their condition in follow-up sessions after the study had ended. (50)
Ibogaine Sustainability Concerns

The primary resource for ibogaine is the iboga plant (tabernanthe iboga), an indigenous shrub of Gabon and other parts of Central and Western Africa. The iboga plant faces a critical threat due to unregulated cultivation for international use. The rise in popularity of ibogaine treatments around the world has led to increased demand for the shrub, and more of it is being exported than is suitable for sustainable growth.
The Gabonese population has used the iboga plant for ceremonial and religious practices, as well as in various medicinal practices, for centuries. The current boom in ibogaine in the Western world has raised concerns for the Gabon people’s culture, and conservation efforts are already underway.
The increased popularity may also be leading to increased health complications, says Lee White, Gabon’s minister of water, forests, the sea, and the environment. Medical-grade ibogaine extracted from iboga root bark can cost up to $150,000 a kilogram. This has led those wishing to make a profit from the plant to cut the ibogaine with bark from another plant, Rauvolfia vomitoria. As its name suggests, Rauvolfia vomitoria is highly toxic, and its deliberate contamination in ibogaine has led to several deaths in the Bwiti religion.(51)
Organizations such as Blessings of The Forest seek to achieve a sustainable future for the iboga plant that not only offers wider availability on a global scale but also protects the way of life of Gabonese and other Central African people. They report that while iboga and ibogaine traders report sustainable conservation, the majority of iboga is still sourced from wild harvesting. This has led to organizations like Conservation Justice and ICEERS campaigning for increased sustainability measures around iboga cultivation and the support of Gabonese culture. Some manufacturers of iboga medicines are now cultivating the plant outside of Gabon in Ghana, Cameroon, and the Ivory Coast as well as suitable regions in Mexico, Brazil, and Costa Rica. (52)(53)
Ibogaine Side Effects & Risks
The positive effects of ibogaine have been well-documented and range from beneficial emotional and behavioral insights to withdrawal-suppressing qualities to addictive substances.
However, there have been studies that suggest the toxicity of the iboga plant can lead to health complications, especially in those with pre-existing heart conditions. It can also cause emotional distress in those less experienced with psychedelics or those with a negative mindset. (54)
Positive Effects
Ibogaine has positive effects that range from deep emotional introspection to vivid closed-eye hallucinations. An ibogaine experience is often more intense and potentially uncomfortable than other psychedelics, but is said to have a profoundly beneficial impact on an individual’s life. (54,55,56)
Positive Effects of Ibogaine
Ibogaine’s Physical Effects and Risks
There are a range of physical side effects that can be potentially harmful to the individual and affect the positivity of the experience if unprepared. Ibogaine has also been linked to cardiovascular issues in certain individuals, meaning it is important to have a medical screening beforehand as well as having someone with medical training on hand during the experience. Most physical effects will begin within 1-3 hours of administration and will subside within 72 hours. More severe side effects can lead to serious health complications that can require medical attention. (57, 54)
Ibogaine Short-Term Side Effects
Severe Physical Effects
Psychological and Emotional Effects
Ibogaine is notorious for its powerful emotional insights and degree of self-reflection. While this can be a positive experience for some, going into an ibogaine journey while in a poor mental mindset or with unmanaged psychological issues can lead to negative outcomes.
Psychological and Emotional Risks of Ibogaine
Contraindications
There are many health risks associated with ibogaine use as well preexisting health conditions that can lead to complications when ibogaine is taken. The most widely reported are cardiovascular and psychiatric contraindications, though there are others to consider. There are also certain medications that should be avoided. (57) (58)
Heart Conditions
The biggest physical risk of ibogaine therapy is its effects on the heart. Noribogaine, the metabolite of ibogaine, blocks potassium ion channels (Kv11.1) in the heart that regulate a normal heart rhythm. This can lead to a life-threatening arrhythmia condition called Torsades de pointes. Kv11.1 channels can also be inhibited by certain medications such as antiarrhythmics, anti-psychotics, and some antibiotics. (57)
It is therefore often mandatory to have potassium ion checked (detected as a prolonged QT-interval or the time between ventricular depolarisation and repolarisation) via an electrocardiogram (ECG) before seeking ibogaine treatment. A long QT interval (which may lead to fatal arrhythmia if affected by ibogaine) may be caused by inherent genetic conditions (congenital heart defects), medications, malnourishment, loss of electrolytes, and chronic cardiovascular diseases. (57)
Almost all cases of recorded fatalities from ibogaine use are related to chronic illnesses or contraindicated medications that already affect the QT level. It is therefore strongly advised that you undergo an ECG and discuss the results with your doctor before attempting ibogaine therapy. Other heart conditions that are considered contraindications for ibogaine include: (59, 58)
Physiological and psychological contraindications
In addition to heart complications, there is a range of conditions that should be monitored or checked for contraindication before seeking ibogaine therapy. The presence of one or more of these conditions may lead to the treatment administrator being unable to fulfill ibogaine therapy for you. (58)
Psychiatric conditions, including:
Respiratory conditions, including:
Severe or chronic gastrointestinal issues, including:
Other conditions or circumstances, including:
Medication contraindications
Any medication that alters the QT interval in the heart or that alters the metabolism of noribogaine can be considered a contraindication for ibogaine. This includes: (60) (61)
Those seeking ibogaine treatment for opioid or stimulant use disorders (such as heroin or cocaine addiction) may also need to taper their intake before treatment as these substances can affect metabolism. (62)
Common FAQs About Ibogaine
Does ibogaine show up on drug tests?
Ibogaine does not share similar metabolites to commonly-tested substances and there are no urine or blood test kits available on the market. This means positive or false positive results for ibogaine are extremely unlikely.
Can you overdose on ibogaine?
There has been extensive research into ibogaine’s effect on the cardiovascular system and the connection between ibogaine and cardiopulmonary arrest, which has been related to over 30 deaths. It is vital that a full medical screening be performed before taking ibogaine and that a healthcare professional be in attendance during the experience. (58)
Sources

1. Fernandez, J. W. (1982). Bwiti: An Ethnography of the Religious Imagination in Africa [Review of Bwiti: An Ethnography of the Religious Imagination in Africa]. Princeton University Press. https://press.princeton.edu/books/hardcover/9780691656656/bwiti (Original work published 1982)
2. Fernandes-Nascimento, M. H., Negrão, A. B., Viana-Ferreira, K., Chaves, B. D. R., & Wang, Y.-P. (2023). Three Decades of Research on the Development of Ibogaine Treatment of Substance Use Disorders: A Scientometric Analysis. Journal of Psychoactive Drugs, 1–11. https://doi.org/10.1080/02791072.2023.2276230
3. Prueger, S. (2021, April 23). What Does Ibogaine Feel Like and How Long Does it Last? Psychable. https://psychable.com/iboga-ibogaine/what-does-ibogaine-feel-like-and-how-long-does-it-last#The-Acute-Experience
4. Opioids. (n.d.). IBOGAINE SAFETY GUIDELINES. Retrieved January 8, 2024, from https://ibogaineguidelines.com/clinical-guidelines/opioids/
5. Popik, P., & Skolnick, P. (1999, January 1). Chapter 3 – Pharmacology of Ibogaine and Ibogaine-Related Alkaloids (G. A. Cordell, Ed.). ScienceDirect; Academic Press. https://www.sciencedirect.com/science/article/abs/pii/S0099959808600279
6. Corkery, J. M. (2018, January 1). Chapter 8 – Ibogaine as a treatment for substance misuse: Potential benefits and practical dangers (T. Calvey, Ed.). ScienceDirect; Elsevier. https://www.sciencedirect.com/science/article/pii/S0079612318300979
7. Efange, S. M. N. (2002, January 1). Chapter 5 – Natural products: a continuing source of inspiration for the medicinal chemist (M. M. Iwu & J. C. Wootton, Eds.). ScienceDirect; Elsevier. https://www.sciencedirect.com/science/article/abs/pii/S1572557X02800149
8. Obembe, S. B. (2012, January 1). 6 – Pharmacotherapy (Medication Therapy) (S. B. Obembe, Ed.). ScienceDirect; Elsevier. https://www.sciencedirect.com/science/article/abs/pii/B9780123985187000067
9. Context of Care. (n.d.). IBOGAINE SAFETY GUIDELINES. Retrieved January 8, 2024, from https://ibogaineguidelines.com/clinical-guidelines/context-of-care/
10. Camlin, T. J., Eulert, D., Thomas Horvath, A., Bucky, S. F., Barsuglia, J. P., & Polanco, M. (2018). A phenomenological investigation into the lived experience of ibogaine and its potential to treat opioid use disorders. Journal of Psychedelic Studies, 2(1), 24–35. https://doi.org/10.1556/2054.2018.004
11. Schenberg, E. E., de Castro Comis, M. A., Alexandre, J. F. M., Tófoli, L. F., Chaves, B. D. R., & da Silveira, D. X. (2017). A phenomenological analysis of the subjective experience elicited by ibogaine in the context of a drug dependence treatment. Journal of Psychedelic Studies, 1(2), 74–83. https://doi.org/10.1556/2054.01.2017.007
12. Introduction. (n.d.). IBOGAINE SAFETY GUIDELINES. Retrieved January 8, 2024, from https://ibogaineguidelines.com/clinical-guidelines/introduction/
13. A New Perspective: My Experience with Ibogaine Treatment. (2015, November 24). Multidisciplinary Association for Psychedelic Studies – MAPS. https://maps.org/news/bulletin/a-new-perspective-my-experience-with-ibogaine-treatment/
14. Camlin, T. J., Eulert, D., Thomas Horvath, A., Bucky, S. F., Barsuglia, J. P., & Polanco, M. (2018). A phenomenological investigation into the lived experience of ibogaine and its potential to treat opioid use disorders. Journal of Psychedelic Studies, 2(1), 24–35. https://doi.org/10.1556/2054.2018.004
15. Prueger, S. (2021, April 12). Ibogaine Integration and Aftercare for Addiction. Psychable. https://psychable.com/addiction/ibogaine-integration-and-aftercare-for-addiction
16. Levi. (2020, January 12). 10 Tips for Integration After An Iboga Retreat. IBOGA. https://ibogawellness.com/post-iboga-integration/
17. Weiss, S. (2021, January 19). Here’s What’s Missing From Conversations About Psychedelic Integration. DoubleBlind Mag. https://doubleblindmag.com/heres-whats-missing-from-conversations-about-psychedelic-integration/
18. Deevoy, R. (2022, September 26). The Messy Job of a Psychedelic Integration Coach. Psychedelic Spotlight. https://psychedelicspotlight.com/the-messy-job-of-a-psychedelic-integration-coach/
19. Knuijver, T., Schellekens, A., Belgers, M., Donders, R., Oosteren, T., Kramers, K., & Verkes, R. (2021). Safety of ibogaine administration in detoxification of opioid‐dependent individuals: a descriptive open‐label observational study. Addiction. https://doi.org/10.1111/add.15448
20. Cherian, K.N., Keynan, J.N., Anker, L. et al. Magnesium–ibogaine therapy in veterans with traumatic brain injuries. (2024). Nat Med 30. https://doi.org/10.1038/s41591-023-02705-w
21. Mash, D. C., Duque, L., Page, B., & Allen-Ferdinand, K. (2018). Ibogaine Detoxification Transitions Opioid and Cocaine Abusers Between Dependence and Abstinence: Clinical Observations and Treatment Outcomes. Frontiers in Pharmacology, 9. https://doi.org/10.3389/fphar.2018.00529
22. Schenberg, E. E., de Castro Comis, M. A., Chaves, B. R., & da Silveira, D. X. (2014). Treating drug dependence with the aid of ibogaine: A retrospective study. Journal of Psychopharmacology, 28(11), 993–1000. https://doi.org/10.1177/0269881114552713
23. Koenig, X., & Hilber, K. (2015). The Anti-Addiction Drug Ibogaine and the Heart: A Delicate Relation. Molecules, 20(2), 2208–2228. https://doi.org/10.3390/molecules20022208
24. Health & Optimization Treatment Program | Beond. (n.d.). Beond WordPress. Retrieved January 8, 2024, from https://beondibogaine.com/health-optimization-program/
25. Ibogaine for Personal Development. (n.d.). Ibogaine Treatment for Addiction. Retrieved January 8, 2024, from https://anzelmoibogaine.com/ibogaine-treatment/personal-development/
26. Adam, Eve and Iboga. (n.d.). Ibogaine. https://ibogaine.mindvox.com/articles/adam-eve-iboga/
27. Samorini/buiti. (n.d.). Www.samorini.it. Retrieved November 1, 2023, from https://www.samorini.it/doc1/sam/bui_int.htm
28. Griffon du Bellay, 1865, Le Gabon, Le Tour du monde, II, 1865, p. 273-379
29. Henri Baillon. (1886). Histoire des plantes.
30. Hevesi, D. (2010, February 17). Howard Lotsof Dies at 66; Saw Drug Cure in a Plant. The New York Times. https://www.nytimes.com/2010/02/17/us/17lotsof.html
31. United States Drug Enforcement Administration. (2018, July 25). The Controlled Substances Act. https://www.dea.gov/sites/default/files/drug_of_abuse.pdf https://www.dea.gov/drug-information/csa
32. R&D Medicines > Ibogaine for Drug Addiction. Multidisciplinary Association for Psychedelic Studies website. Available at: www.maps.org/ibogaine/
33. Alper KR, Glick SD, eds. Ibogaine: Proceedings from the First International Conference. San Diego, CA: Academic Press; 2001.
34. Pullen, J. (2023, May 4). A trip to West Africa: Gabon’s indigenous psychedelic [Review of A trip to West Africa: Gabon’s indigenous psychedelic]. British Pharmacological Society. https://www.bps.ac.uk/publishing/pharmacology-matters/may-2023/a-trip-to-west-africa;-gabon%e2%80%99s-indigenous-psychede
35. Glick, S. D., Et Al. (2000). 18-Methoxycoronaridine (18-MC) and Ibogaine: Comparison of Antiaddictive Efficacy, Toxicity, and Mechanisms of Action. Annals of the New York Academy of Sciences, 914(1), 369–386. https://doi.org/10.1111/j.1749-6632.2000.tb05211.x
36. Koenig, X., & Hilber, K. (2015). The Anti-Addiction Drug Ibogaine and the Heart: A Delicate Relation. Molecules, 20(2), 2208–2228. https://doi.org/10.3390/molecules20022208
37. Love, B. (2019, March 10). Losing the Plant that Treats Addiction: The Strange History of the Ibogaine Movement in the United States – Britta Love. https://brittaloved.com/how-we-almost-cured-addiction-the-strange-history-of-the-ibogaine-movement-in-the-united-states/
38. Glick, S. D., Kuehne, M. E., Maisonneuve, I. M., Bandarage, U. K., & Molinari, H. H. (1996). 18-Methoxycoronaridine, a non-toxic iboga alkaloid congener: effects on morphine and cocaine self-administration and on mesolimbic dopamine release in rats. Brain Research, 719(1-2), 29–35. https://doi.org/10.1016/0006-8993(96)00056-x
39. Kentucky Opioid Abatement Advisory Commission hears from public on funding for ibogaine research. (2023, September 18). WEKU. https://www.weku.org/the-commonwealth/2023-09-18/kentucky-opioid-abatement-advisory-commission-hears-from-public-on-funding-for-ibogaine-research
40. Kentucky’s $42m Ibogaine Funding Appears Dead in the Water. (2023, December). Psychedelic Alpha. https://psychedelicalpha.com/news/kentuckys-42m-ibogaine-funding-appears-dead-in-the-water
41. Ibogaine Legality by Country 2023. (n.d.). Worldpopulationreview.com. Retrieved November 1, 2023, from https://worldpopulationreview.com/country-rankings/ibogaine-legality-by-country
42. 13 Red Flags for Ibogaine Treatment: Psychable helps show you how to avoid dangerous treatment. (n.d.). Psychable. Retrieved January 8, 2024, from https://psychable.com/press/13-red-flags-for-ibogaine-treatment-psychable-helps-show-you-how-to-avoid-dangerous-treatment
43. Levi. (2020, January 12). 10 Tips for Integration After An Iboga Retreat. IBOGA. https://ibogawellness.com/post-iboga-integration/
44. Weiss, S. (2021, January 19). Here’s What’s Missing From Conversations About Psychedelic Integration. DoubleBlind Mag. https://doubleblindmag.com/heres-whats-missing-from-conversations-about-psychedelic-integration/
45. Deevoy, R. (2022, September 26). The Messy Job of a Psychedelic Integration Coach. Psychedelic Spotlight. https://psychedelicspotlight.com/the-messy-job-of-a-psychedelic-integration-coach/
46. Knuijver, T., Schellekens, A., Belgers, M., Donders, R., Oosteren, T., Kramers, K., & Verkes, R. (2021). Safety of ibogaine administration in detoxification of opioid‐dependent individuals: a descriptive open‐label observational study. Addiction. https://doi.org/10.1111/add.15448
47. Iboga Uses, Benefits & Dosage – Drugs.com Herbal Database. (n.d.). Drugs.com. https://www.drugs.com/npp/iboga.html
48. Ibogaine. (n.d.). New Scientist. Retrieved January 8, 2024, from https://www.newscientist.com/definition/ibogaine/
49. How to Microdose Drugs Based On What You’re Using. (n.d.). Www.vice.com. https://www.vice.com/en/article/xgdpan/what-is-microdosing-psychedelic-mushrooms-lsd-drugs-guide-effects-benefits-risks
50. Fernandes-Nascimento, M. H., Viana-Ferreira, K., Chaves, B. D. R., Negrão, A. B., & Wang, Y.-P. (2022). Ibogaine microdosing in a patient with bipolar depression: a case report. Brazilian Journal of Psychiatry. https://doi.org/10.47626/1516-4446-2021-2359
51. Sullivan, K. (2023, January 24). The psychedelic ibogaine can treat addiction. The race is on to cash in. The Guardian. https://www.theguardian.com/society/2023/jan/23/ibogaine-iboga-drug-addiction-psychedelic-gabon
52. Blessings of The Forest. (n.d.). Retrieved November 1, 2023, from https://blessingsoftheforest.org/
53. Iboga Conservation. (2021, June 7). Chacruna. https://chacruna.net/iboga_conservation/
54. What is ibogaine and what are the effects, dosage, and risks? – Drug Science. (n.d.). Drugscience.org.uk. Retrieved November 1, 2023, from https://www.drugscience.org.uk/drug-information/ibogaine/#1612864461102-f2986b30-ab15
55. Iboga Uses, Benefits & Dosage – Drugs.com Herbal Database. (n.d.). Drugs.com. https://www.drugs.com/npp/iboga.html
56. Davis, A. K., Averill, L. A., Sepeda, N. D., Barsuglia, J. P., & Amoroso, T. (2020). Psychedelic Treatment for Trauma-Related Psychological and Cognitive Impairment Among US Special Operations Forces Veterans. Chronic Stress, 4, 247054702093956. https://doi.org/10.1177/2470547020939564
57. Koenig, X., Kovar, M., Boehm, S., Sandtner, W., & Hilber, K. (2014). Anti-addiction drug ibogaine inhibits hERG channels: a cardiac arrhythmia risk. Addiction biology, 19(2), 237–239. https://doi.org/10.1111/j.1369-1600.2012.00447.x
58. Patient Criteria & Considerations. (n.d.). IBOGAINE SAFETY GUIDELINES. Retrieved January 17, 2024, from https://ibogaineguidelines.com/clinical-guidelines/patient-criteria-considerations/
59. Glue, P., Lockhart, M., Lam, F., Hung, N., Hung, C. T., & Friedhoff, L. (2015). Ascending-dose study of noribogaine in healthy volunteers: pharmacokinetics, pharmacodynamics, safety, and tolerability. Journal of clinical pharmacology, 55(2), 189–194. https://doi.org/10.1002/jcph.404
60. Papadodima, S. A., Dona, A., Evaggelakos, C. I., Goutas, N., & Athanaselis, S. A. (2013). Ibogaine related sudden death: a case report. Journal of forensic and legal medicine, 20(7), 809–811. https://doi.org/10.1016/j.jflm.2013.06.032
61. Ereshefsky, L., Riesenman, C., & Lam, Y. W. (1995). Antidepressant drug interactions and the cytochrome P450 system. The role of cytochrome P450 2D6. Clinical pharmacokinetics, 29 Suppl 1, 10–19. https://doi.org/10.2165/00003088-199500291-00004
62. Nachimuthu, S., Assar, M. D., & Schussler, J. M. (2012). Drug-induced QT interval prolongation: mechanisms and clinical management. Therapeutic advances in drug safety, 3(5), 241–253. https://doi.org/10.1177/2042098612454283

 Edmund Murphy
Edmund Murphy Morgan Blair, MA, LPC
Morgan Blair, MA, LPC Paloma Lehfeldt, MD
Paloma Lehfeldt, MD





 Stephanie Karzon
Stephanie Karzon Nir Tadmor
Nir Tadmor Ben “Doc” Askins
Ben “Doc” Askins Sofie Mikhaylova
Sofie Mikhaylova David Connell
David Connell



 Lauren Smith
Lauren Smith
