In this week’s Psychedelic News Roundup, an opinion piece published by the Washington Post, has the psychedelic community in an uproar. Responses from leaders in the field have triggered a firestorm of indignation from the wider psychedelic community, with experts like Michael Pollan and Robin Carhart-Harris taking fire from psychedelic enthusiasts on social media. Other news includes increased interest in psychedelics among the clergy, new DMT study results from Cybin Inc., and the raid of a Detroit-based Psychedelic Church.
The Risks of Self-Medicating with Psychedelics: A Passionately Debated Opinion

A recent opinion piece in the Washington Post has been stirring controversy. Jonathan Alpert, Chairman of the Albert Einstein College of Medicine, recently contributed to the article by Leana S. Wen, detailing what they consider to be significant risks and dangers associated with self-medicating using psychedelics.
The piece essentially argues that psychedelics, such as psilocybin and MDMA, have shown significant potential in treating mental health disorders in controlled studies. However, as these substances become more available, there’s growing concern that individuals might self-medicate, bypassing evidence-based therapies. The FDA is currently reviewing studies on these drugs for treating severe depression and PTSD. Recent clinical trials have shown promising results, with psilocybin combined with psychotherapy leading to a sustained reduction in depressive symptoms and MDMA-assisted therapy helping 71% of PTSD patients no longer meet the criteria for the disorder.
However, the piece says, these studies have limitations. Jonathan Alpert, chair of the Department of Psychiatry and Behavioral Sciences at the Albert Einstein College of Medicine, points out that the sample sizes are small, with the psilocybin study involving only 51 patients and the MDMA study having 53. Moreover, participants were carefully screened, excluding those with recent suicidal thoughts, certain behavioral health conditions, or even immediate family members with psychotic disorders. Alpert emphasizes the risks, noting that some recreational users have experienced long-term consequences like psychosis, mania, and depression.
Keep Up with Uncensored Psychedelic Trends
Join our newsletter at Psychedelics Uncensored.
We respect and protect your privacy. By subscribing your info will be subject to our privacy policy . Unsubscribe easily at any time
The concern stated by the author is that without proper safeguards, these drugs might be misused by those at high risk for dangerous side effects. The studies required participants to undergo extensive preparatory sessions, supervised dosing sessions, and post-administration therapy. Alpert has encountered patients who’ve tried psychedelics sourced from friends instead of seeking mental health treatment, highlighting the dangers of self-medication. He stresses that those opting for psychedelics should be under the care of trained professionals throughout their therapy.
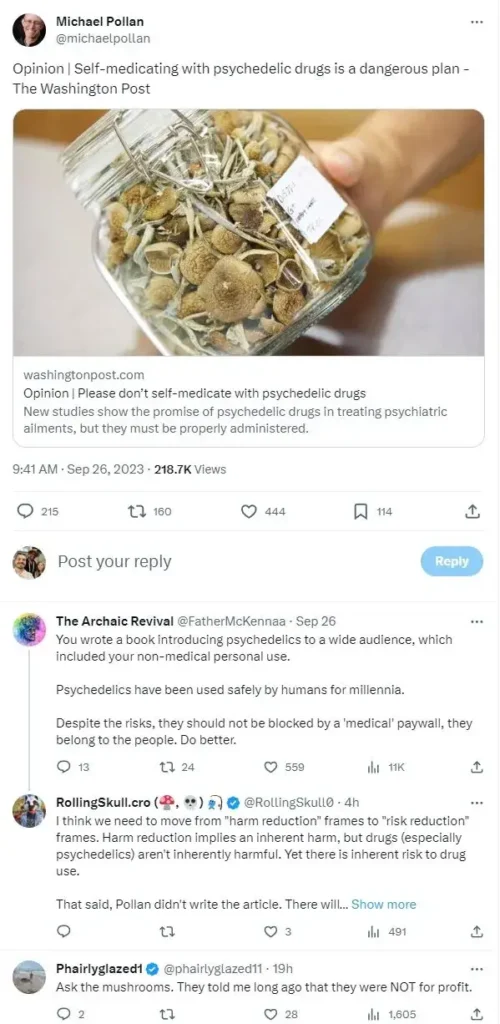
Wen concludes by drawing parallels between self-medicating with psychedelics and self-treating other medical conditions. Just as one wouldn’t self-administer chemotherapy or bypass the FDA’s approval process for heart medications, the same caution should apply to psychedelics. The increasing trend of self-medicating with these drugs reflects the stigma around mental health. Wen argues that mental health disorders should be treated with the same rigor and evidence-based care as physical ailments, emphasizing the potential harm to those who self-medicate without understanding the risks.(1)
Leaders in the field came out in support of Wen’s article. With Robin Carhart-Harris and Michael Pollan both agreeing. Carhart-Harris, a leading psychedelic researcher at the Centre for Neuropsychopharmacology at Imperial College London, had this to say on X, formerly Twitter, “I tend to agree. It’s too easy for it to be done badly and for things to go (potentially seriously) wrong.” Another leader in the field, Michael Pollan, author of several books on psychedelics, including his most recent entry, the Psychedelic Handbook, also offered their support. Pollan, in particular, took fire from fans displeased by his stance, with some accusing Pollan of hypocrisy and gatekeeping.
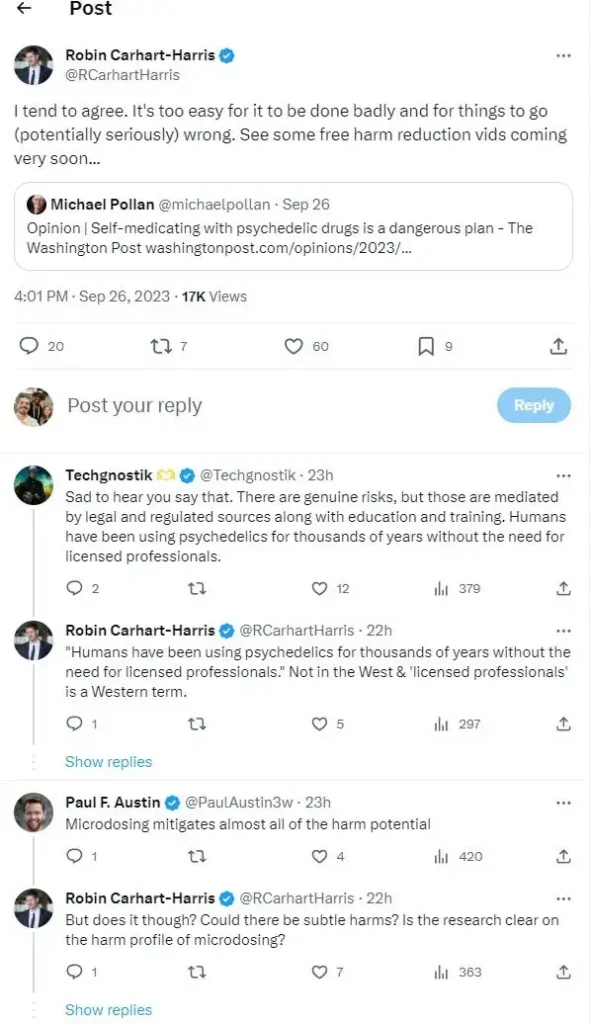
One of the community’s most common concerns involves cost and accessibility. Many users pointed to the high cost of medical-only psychedelic use, highlighting Oregon’s psilocybin access program allowing for supervised adult use. These supervised sessions can run as high as $3,400 and are not covered by insurers. Others offered their personal experiences using psychedelics to self-treat conditions like PTSD, with many claiming that experts like Pollan and Carhart-Harris inspired them to explore psychedelics. Interestingly, the Oregon program, often used as an example of psychedelic-assisted therapy, does not, in fact, allow for psilocybin to be used for medical purposes.
Some individuals considered microdosing (the practice of taking sub-perceptual doses of psychedelics) a foolproof and safe way to self-medicate. Carhart-Harris quickly refuted this, offering that in his expert opinion that the research is not yet fully developed and caution is warranted.
Another concern is the disenfranchisement of traditional and underground psychedelic leaders. The medical-only approach to psychedelics fails to account for indigenous communities’ psychedelic medicine and spiritual traditions dating back thousands of years. It also dismisses the role of underground psychedelic leaders and facilitators, many of whom have decades of experience, in favor of trained clinicians, who may have limited first-hand experience with psychedelics and far fewer years of experience as guides.
Keep Up with Psychedelic Trends
Get uncensored psychedelic news, events, and updates. Join Psychedelics Uncensored!
We respect and protect your privacy. By subscribing your info will be subject to our privacy policy . Unsubscribe easily at any time
Chaplains Explore the Intersection of Psychedelics and Spirituality

Originally published by NPR, research into the therapeutic potential of psychedelics is expanding, with studies indicating their efficacy in treating conditions like PTSD and depression. As regulatory models emerge in states like Oregon and Colorado, a unique group is showing interest in this field: chaplains. These religious professionals, who work in secular environments like hospitals and schools, are trained to guide individuals through profound life moments, regardless of their faith or lack thereof.
Caroline Peacock, an Episcopal priest and director of spiritual health at Emory University’s Winship Cancer Institute, participated in a clinical trial using psilocybin on terminal cancer patients. Chaplains in this study collaborated with mental health experts during the drug administration and subsequently helped patients integrate their experiences. Recognizing the potential of this intersection, Peacock initiated the Psychedelic Care Network within the Transforming Chaplaincy think tank, attracting over 150 chaplains. The interest is evident as major chaplain associations have held workshops and discussions on psychedelic-assisted therapy.
Many are drawn to this field because psychedelics often induce what’s described as a mystical experience. Clinical psychologist Anthony Bossis, who has conducted psilocybin trials at NYU Grossman School of Medicine, notes that patients describe feelings of awe, interconnectedness, and transcendence. The spiritual aspect of the psychedelic experience appears to enhance the therapeutic outcomes. Bossis mentions that these experiences can significantly reduce depression, anxiety, and fear of death among patients with advanced illnesses.
Religious traditions, such as Ayahuasca ceremonies in South America and peyote rituals in Mexico, have long centered around psychedelics. However, other religions are now finding ways to contextualize these experiences. Jaime Clark-Soles, a New Testament scholar, participated in a psilocybin trial for religious professionals at Johns Hopkins University. She felt a profound connection with God during her experience and is now training to facilitate psychedelic-assisted therapy. While some critics argue that these experiences are drug-induced and not genuinely spiritual, Clark-Soles counters that context shapes all spiritual encounters. The ultimate measure, she suggests, is the impact on individuals’ lives. As the boundaries between religion and psychedelics blur, chaplains aim to merge their expertise with these transformative experiences, assisting those grappling with life’s profound questions.(2)
Psychedelics in Pain Management: A Preliminary Review

In a new study published in Anesthesiology, researchers explore the psychedelic potential for pain management. Chronic pain, affecting around 1.5 billion people worldwide, is a significant public health issue. Traditional treatments, including both opioid and non-opioid analgesics, often come with side effects, addiction risks, and sometimes ineffective pain relief. This has led to a search for alternative therapeutic agents that can address chronic pain through different mechanisms. Psychedelics, such as lysergic acid diethylamide (LSD) and psilocybin (found in psychedelic mushrooms), are believed to modify pain perception. They achieve this through direct serotonin receptor activation, anti-inflammatory actions, and changes in synaptic structures.
A scoping review was undertaken by Akash Goel, M.D., M.P.H., and colleagues to pinpoint human studies where psychedelic substances were employed to treat pain. Out of the studies identified, 21 articles were included that evaluated the impact of psychedelics on various pain conditions. However, the limited number of clinical trials and the small sample sizes in existing studies restrict their immediate clinical application.
The preliminary findings suggest that psychedelics might be beneficial in providing pain relief, particularly for specific headache disorders and cancer-related pain. To better understand the potential of psychedelics in pain management, future research should focus on the combined influence of psychotherapy and psychedelics on chronic pain.(3)
Promising Results from DMT-SSRI Drug Interaction Study for Depression

Cybin Inc., a clinical-stage biopharmaceutical company, announced the results of a study conducted in partnership with Small Pharma Inc. The results represent positive data from a Phase Ib study that investigated the interaction between selective serotonin reuptake inhibitors (SSRIs) and SPL026, a native N, N-dimethyltryptamine (DMT), in patients with Major Depressive Disorder (MDD). This comes as Cybin is set to acquire Small Pharma Inc. in an all-share transaction expected to close in Q4 2023.
The study involved 171 patients, with 12 in the SSRI Cohort (on SSRIs) and 5 in the Non-SSRI Cohort (not on any pharmacological treatment for depression). Efficacy was measured using the Montgomery-Asberg Depression Rating Scale (MADRS) and the Beck Depression Inventory (BDI).
The study aimed to determine if SPL026 (DMT) can be safely administered with or without SSRIs, the current standard treatment for MDD. Previously, patients had to be withdrawn from SSRIs, which could be disruptive. The recent study addressed this, potentially facilitating broader patient recruitment for future studies and possibly speeding up the clinical development pathway.
Key Findings:
- SPL026 was well-tolerated by all patients in both cohorts.
- No drug-related serious adverse events were reported.
- At Week 4, 100% of patients in the SSRI cohort responded to SPL026, with 92% in remission from depression.
- The results suggest that SSRIs enhance the efficacy of SPL026, indicating a potentially enhanced therapeutic effect when combined with SSRIs.
Doug Drysdale, CEO of Cybin, expressed excitement over the new data, emphasizing the potential synergistic power of their combined programs. Dr. Carol Routledge, Chief Medical and Scientific Officer of Small Pharma, highlighted the unexpected marked difference in efficacy when administering SPL026 with SSRIs compared to SPL026 alone. George Tziras, CEO of Small Pharma, emphasized the potential of delivering a DMT-based treatment to patients on SSRIs (that do not adequately alleviate their depression symptoms).
The study indicates that combining SPL026 with SSRIs might offer enhanced therapeutic benefits for MDD patients, presenting a compelling case for its early inclusion in the treatment pathway.(4)
Detroit’s “Psychedelic Church” Raided Over Mushroom Distribution

Coming to us from Fox 2 Detroit, Detroit’s self-proclaimed “Psychedelic Church,” Soul Tribes International Ministries, was recently raided by the city’s police due to its distribution of Psilocybin (aka magic mushrooms). The church’s leader, Robert Shumake, known as “Shaman Shu,” believes he was targeted by the city and police for offering mushrooms, which he refers to as “sacred plants,” to his congregation.
Shaman Shu asserts that his primary goal is to aid individuals in addressing and improving their mental health. He emphasizes the role of a shaman in helping people identify and understand their trauma, including generational or ancestral trauma. In 2021, he claimed to have played a role in creating “Prop E,” an ordinance that decriminalized the use of mushrooms in Detroit. Following its approval by voters, he opened his church in March.
However, city officials argue that despite the local ordinance, state law still classifies psilocybin (the active compound in mushrooms) as a controlled substance. The city’s attorney, Doug Baker, clarified that the ordinance does not supersede state law nor permit the sale or distribution of psilocybin. Consequently, the activities at Shaman Shu’s church are considered illegal under Michigan law.
What Is a Shaman? Learn the Origins of Shamanism and How We’ve Been Using This Word Wrong All Along.
Shaman Shu counters this by emphasizing his mission to steer people away from harmful street drugs like Percocet, oxycontin, and fentanyl. He advocates for the therapeutic potential of “sacred sacraments” and is currently assembling a legal team to challenge the shutdown and reopen his church.(5)
Sources

1. Wen, L. S. (2023, September 26). Opinion | Please don’t self-medicate with psychedelic drugs. Washington Post. https://www.washingtonpost.com/opinions/2023/09/26/psychedelics-mental-health-treatment-depression-ptsd/
2. As psychedelic-assisted therapy grows, so does interest from a new group: chaplains. (2023, September 24). NPR. https://www.npr.org/2023/09/24/1201095225/as-psychedelic-assisted-therapy-grows-so-does-interest-from-a-new-group-chaplain
3. Goel, A., Rai, Y., Shayan Sivadas, Diep, C., Clarke, H., Harsha Shanthanna, & Ladha, K. (2023). Use of Psychedelics for Pain: A Scoping Review. Anesthesiology, 139(4), 523–536. https://doi.org/10.1097/aln.0000000000004673
4. Cybin – Small Pharma Reports Positive Top-line Data from SPL026 (DMT)-SSRI Drug Interaction Study in Patients with Major Depressive Disorder. (n.d.). Ir.cybin.com. Retrieved September 27, 2023, from https://ir.cybin.com/investors/news/news-details/2023/Small-Pharma-Reports-Positive-Top-line-Data-from-SPL026-DMT-SSRI-Drug-Interaction-Study-in-Patients-with-Major-Depressive-Disorder/default.aspx
5. Hudson, B. (2023, September 26). Psychedelic church that gives members mushrooms raided by Detroit police. FOX 2 Detroit. https://www.fox2detroit.com/news/psychedelic-church-that-gives-members-mushrooms-raided-by-detroit-police
This material is not intended as a replacement or substitute for any legal or medical advice. Always consult a medical professional about your health needs. Psychedelics are widely illegal in the United States, and readers should always be informed about local, state, and federal regulations regarding psychedelics or other drugs.

 David Connell
David Connell
 Ross Dillon
Ross Dillon 
